NHS England’s Big Update: More Local Health Services Explained

Getting the healthcare you need, when you need it, is important for everyone. We all know that sometimes booking a GP appointment can be tricky, and waits can be long. The good news is that the NHS in England is making some significant changes to help with this. A major GP scheme expanded UK initiative is underway, designed to bring NHS care closer to home for millions of people.
This means making it easier and quicker for you to access essential health services right in your local community, often without needing to see a doctor first. Let’s explore what these changes involve and, crucially, how the expanded GP scheme affects patients like you.
What Does “Care Closer to Home” Actually Mean?
The main idea is simple: utilise the skills of highly trained health professionals already working in your community, like pharmacists, opticians (optometrists), and audiologists. By expanding the range of NHS services in community settings, the aim is to provide you with faster, more convenient care for a variety of health needs.
This isn’t about replacing your GP. Your doctor plays a key role in your care, especially for complex or long-term health issues. This plan helps by allowing other trained professionals to manage specific problems, giving GPs more time for serious cases. The goal is to tackle the difficult “8 am scramble” for appointments and ensure that those who urgently need to see a GP can do so more easily. This initiative is a key part of the NHS’s wider “Primary Care Access Recovery Plan” in England.
Your Local Pharmacy: A Hub for More Health Services
One of the biggest changes involves your local pharmacy. Pharmacists are highly trained healthcare professionals, and their role is expanding significantly. The Pharmacy First scheme in the UK is a major part of this transformation.
What is the Pharmacy First Scheme?
Expected to launch fully from Winter 2023-24, this service allows pharmacists to assess and treat patients for seven common health conditions without the need for a GP appointment or prescription. With this focus on treating minor illnesses pharmacy UK aims to make care much more accessible.
The seven conditions covered under Pharmacy First will be:
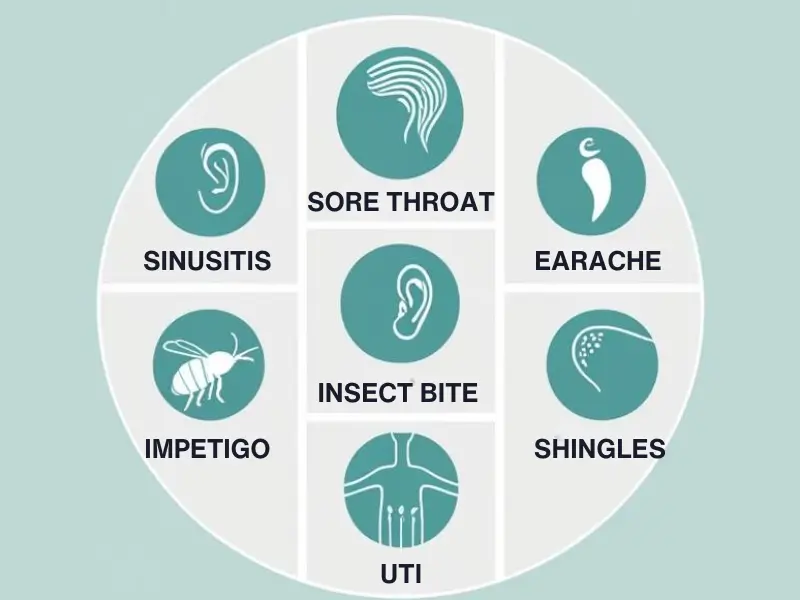
- Sinusitis (for patients aged 12 years and over)
- Sore throat (for patients aged 5 years and over)
- Earache (for patients aged 1 to 17 years)
- Infected insect bites (for patients aged 1 year and over)
- Impetigo (a bacterial skin infection, for patients aged 1 year and over)
- Shingles (for patients aged 18 years and over)
- Uncomplicated urinary tract infections (UTIs) in women (aged 16 to 64 years)
How Can You Use the Pharmacy First Service?
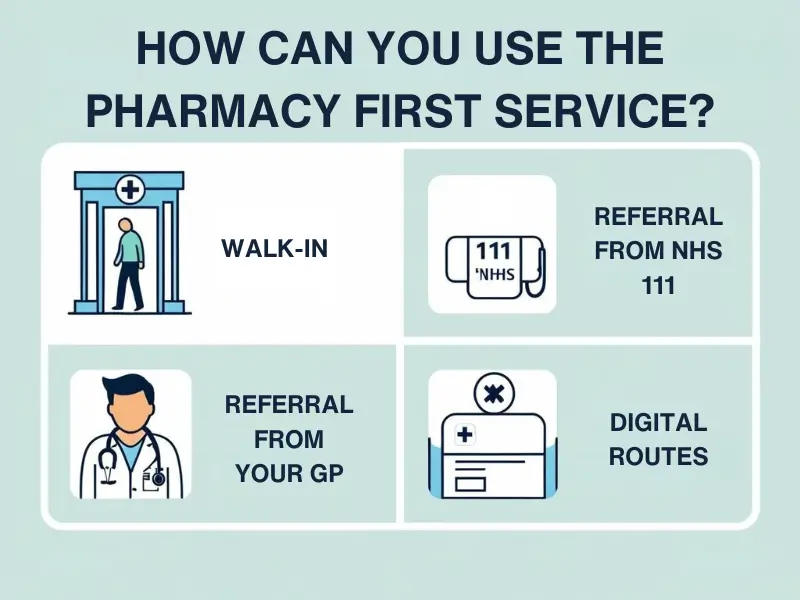
Accessing this service is designed to be straightforward:
- Walk-in: You can often go directly to your local participating pharmacy and ask for advice or treatment for one of these conditions.
- Referral from NHS 111: If you call NHS 111, they might refer you to a local pharmacy.
- Referral from your GP: Your doctor’s surgery might also refer you to the pharmacy.
- Digital Routes: In the future, referrals might also come through digital GP access routes or potentially via the NHS app.
More Than Just Minor Illnesses
Beyond the Pharmacy First scheme, the expansion of community pharmacy services in the NHS includes:
- Blood Pressure Checks: More pharmacies will offer checks for people aged 40 and over, helping to identify high blood pressure early. The aim is to deliver 2.5 million checks a year.
- Oral Contraception: Women will find it easier to get prescriptions for oral contraception directly from their pharmacy, without needing to see a GP first.
The government is investing £645 million over two years to support pharmacies in delivering these expanded services, showing a strong commitment to this new way of working.
Easier Access to Specialist Eye and Ear Checks
It’s not just pharmacies getting enhanced roles. The changes also make it simpler to access checks for specific eye and hearing issues.
Your GP will now be able to refer you directly to other local specialists:
- Optometrists (Opticians): If you have certain eye conditions that need assessment, your GP can refer you straight to a local optician, bypassing the need for a hospital appointment in many cases.
- Audiologists: Similarly, for concerns about hearing loss or other hearing issues, your GP can refer you directly to an audiologist for tests and checks.
This direct referral pathway cuts down on waiting times and extra appointments, getting you the specialist checks you need more efficiently.
Understanding NHS “Advice and Guidance”
You might sometimes hear NHS staff talk about “Advice and Guidance.” What is NHS Advice and Guidance? In simple terms, it’s often an internal process designed to make healthcare more efficient. Instead of automatically sending a patient for a full specialist appointment, which might involve a long wait, GP advice and guidance systems allow a GP to quickly ask for electronic advice from a hospital specialist about the best course of action for a patient.
The specialist can review the case details and provide prompt advice back to the GP, perhaps suggesting a specific test, a medication change, or confirming if a face-to-face specialist appointment is truly necessary. While you might not interact with this system directly, it’s another tool the NHS uses behind the scenes to streamline care, potentially getting you the right treatment plan faster and avoiding unnecessary referrals. It fits into the overall goal of using NHS resources wisely and ensuring you see the right professional at the right time.
What Does This Mean for Your GP?
These changes are designed to support, not replace, your GP. By offering alternatives to GP appointments UK for certain conditions and checks, the expanded scheme aims to:
- Free Up GP Time: The goal is to free up around 10 million GP appointments nationally each year once the schemes are fully running.
- Focus on Complex Needs: GPs can now spend more time with patients who have complex health issues, long-term conditions, or needs that others can’t manage.
- Improve Access: Ultimately, it should make it easier for everyone to get a GP appointment when they genuinely need one.
Your GP practice remains your main point of contact for ongoing care and more serious health concerns.
Technology: Helping to Make Access Smoother
Supporting all these changes is a significant investment in technology. The NHS is putting £240 million into upgrading the digital tools used by GP practices. This includes better online booking systems, improved digital communication, and potentially more features within the NHS App. The aim is to make contacting your practice and accessing services simpler and more convenient for everyone.
How These Changes Benefit You: The Bottom Line
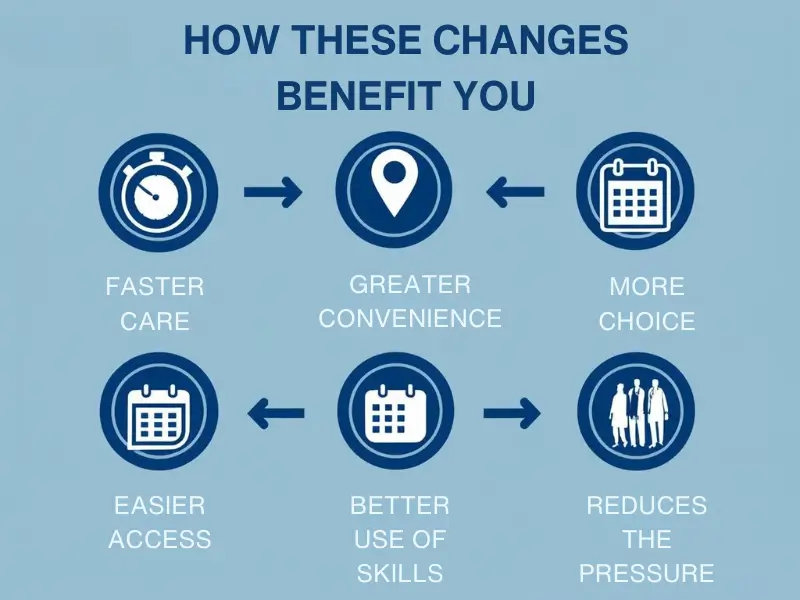
So, how expanded GP scheme affect patients in practical terms? Here are the key benefits you should experience:
- Faster Care: Get assessed and treated more quickly for common conditions at your local pharmacy.
- Greater Convenience: Access essential checks and services closer to where you live or work. No need for unnecessary trips to the GP surgery or hospital for certain issues.
- More Choice: You have more options for where and how you receive care for specific health needs.
- Easier Access: Reduces the pressure on GP appointments, making it easier to see a doctor when you need to.
- Better Use of Skills: Makes the most of the expertise held by pharmacists, opticians, and audiologists in your community.
Important Note: Location
It’s worth remembering that while the overall direction is UK-wide, the specific details outlined here, particularly the “Pharmacy First” scheme with its seven conditions and the direct referral pathways, primarily apply to NHS England as part of their Primary Care Access Recovery Plan. Scotland, Wales, and Northern Ireland may offer slightly different services and schemes, but they often follow similar community care principles.
A More Modern, Accessible NHS
These changes significantly modernise how England delivers primary care. By embracing the skills of community health professionals and investing in technology, the NHS aims to create a system that is more responsive, convenient, and sustainable for the future.
The focus is firmly on making sure you can get the right care, in the right place, at the right time. While it might take a little while for all these services to be fully up and running everywhere, the direction is clear: bringing NHS care closer to home and making healthcare access easier for everyone. Keep an eye out for information from your local GP practice and pharmacy about how you can benefit from these new services as they roll out.
Read more about Mental Health Support for Students in UK Universities
Source / Ref.: Gov.uk Contains public sector information licensed under Open Government Licence v3.0.
Written by [Ketan Borada / British Portal Team] – Founder of British Portal, dedicated to providing accurate and up-to-date information on UK public services and benefits.























